Hypertension—commonly called high blood pressure—is a chronic medical condition in which the force of blood against arterial walls remains persistently elevated above normal levels. Often referred to as the “silent killer,” hypertension typically produces no noticeable symptoms until serious complications develop.
Left untreated, chronic high blood pressure damages vital organs, including the heart, brain, kidneys, eyes, and vascular system, leading to heart attacks, strokes, heart failure, kidney disease, and vision loss.
For nursing students and practicing nurses, understanding how to assess, diagnose, and manage hypertension is essential for preventing life-threatening complications and promoting long-term cardiovascular health.
This comprehensive guide explains the pathophysiology of hypertension, outlines evidence-based nursing assessment techniques, identifies priority NANDA-I nursing diagnoses, and provides five detailed nursing care plans with rationales aligned with the latest NANDA-I 2024–2026 guidelines.
Whether you’re preparing for the NCLEX exam or developing care plans for clinical practice, this article equips you with the foundational knowledge and practical strategies to deliver safe, effective nursing care for patients with hypertension.
- Definition and Overview
- Pathophysiology
- Types of Hypertension
- Causes and Related Factors
- Signs and Symptoms
- Nursing Assessment
- NANDA-I Nursing Diagnoses for Hypertension
- Expected Outcomes and Goals
- Nursing Interventions (General)
- Nursing Care Plans for Hypertension
- Patient and Family Education
- Frequently Asked Questions
- References
Definition and Overview
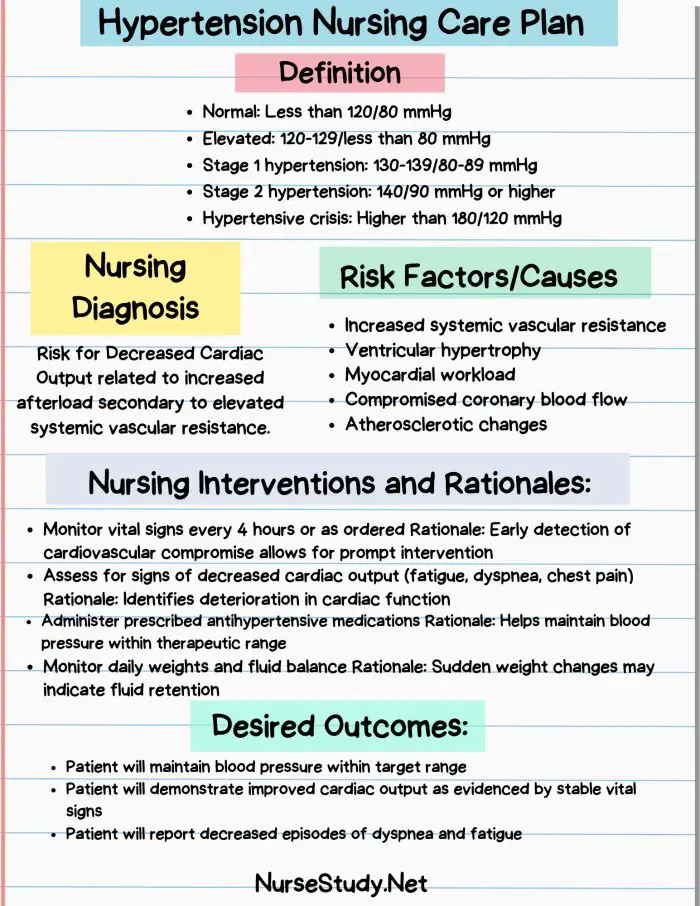
Hypertension is defined as persistently elevated blood pressure readings of ≥130/80 mmHg based on current clinical guidelines. Blood pressure measurements consist of two values: systolic pressure (the pressure when the heart contracts) and diastolic pressure (the pressure when the heart relaxes between beats). According to the 2026 guidelines, hypertension is classified into stages:
- Elevated: Systolic 120–129 mmHg and diastolic <80 mmHg
- Stage 1 Hypertension: Systolic 130–139 mmHg or diastolic 80–89 mmHg
- Stage 2 Hypertension: Systolic ≥140 mmHg or diastolic ≥90 mmHg
- Hypertensive Crisis: Systolic >180 mmHg and/or diastolic >120 mmHg (requires immediate medical intervention)
Hypertension affects approximately half of all U.S. adults and is a leading modifiable risk factor for cardiovascular disease, stroke, chronic kidney disease, and premature death. As nurses, we play a critical role in early detection, patient education, medication management, and lifestyle counseling to reduce the global burden of this condition.
Pathophysiology
How Blood Pressure Is Regulated
Blood pressure is determined by two primary factors: cardiac output (the volume of blood the heart pumps per minute) and systemic vascular resistance (the degree of constriction or dilation in the arterioles). The formula is:
Blood Pressure = Cardiac Output × Systemic Vascular Resistance
Normal blood pressure regulation involves complex interactions between the cardiovascular system, kidneys, autonomic nervous system, and hormonal pathways—particularly the renin-angiotensin-aldosterone system (RAAS).
The Renin-Angiotensin-Aldosterone System (RAAS)
The RAAS plays a central role in blood pressure control and hypertension pathophysiology:
- Renin Release: When blood pressure drops, the kidneys release the enzyme renin into the bloodstream.
- Angiotensin II Formation: Renin converts angiotensinogen (produced by the liver) into angiotensin I, which is then converted to angiotensin II by angiotensin-converting enzyme (ACE) in the lungs.
- Vasoconstriction and Aldosterone Secretion: Angiotensin II causes powerful vasoconstriction (narrowing of blood vessels), raising vascular resistance. It also triggers the adrenal glands to release aldosterone.
- Sodium and Water Retention: Aldosterone promotes sodium and water reabsorption in the kidneys, increasing blood volume and further elevating blood pressure.
In hypertension, the RAAS often becomes overactive, leading to chronic vasoconstriction, increased blood volume, and sustained high blood pressure.
Vascular Changes and Target Organ Damage
Over time, chronic hypertension causes structural and functional changes in blood vessels and organs:
- Arterial Stiffening: Constant high pressure damages the endothelial lining of arteries, causing inflammation, plaque buildup (atherosclerosis), and loss of elasticity.
- Left Ventricular Hypertrophy (LVH): The heart muscle thickens to overcome increased resistance, eventually leading to heart failure if untreated.
- Kidney Damage: High pressure damages the delicate filtering units (nephrons), reducing kidney function and potentially causing chronic kidney disease.
- Retinopathy: Blood vessels in the retina narrow, leak, or hemorrhage, impairing vision.
- Cerebrovascular Disease: Weakened blood vessels in the brain increase stroke risk.
Nurses must assess for signs of target organ damage during initial evaluation and ongoing monitoring, as this significantly impacts treatment decisions and prognosis.
Types of Hypertension
Primary (Essential) Hypertension
Approximately 90–95% of hypertension cases are primary hypertension, meaning no single identifiable cause exists. Instead, multiple genetic, environmental, and lifestyle factors contribute to its development over many years. Primary hypertension typically emerges in adulthood and progresses gradually.
Secondary Hypertension
The remaining 5–10% of cases are secondary hypertension, caused by an underlying medical condition or medication. Common causes include:
- Renal Disease: Chronic kidney disease, polycystic kidney disease, renal artery stenosis
- Endocrine Disorders: Primary aldosteronism, Cushing’s syndrome, pheochromocytoma, hyperthyroidism
- Medications: Oral contraceptives, NSAIDs, corticosteroids, decongestants, certain antidepressants
- Obstructive Sleep Apnea: Repeated episodes of oxygen desaturation and sympathetic activation
- Coarctation of the Aorta: Congenital narrowing of the aorta
Identifying secondary hypertension is important because treating the underlying cause may resolve or significantly improve blood pressure control.
Causes and Related Factors
Multiple risk factors contribute to hypertension development. In NANDA-I nursing diagnosis terminology, these are expressed as “related to” factors:
Non-Modifiable Risk Factors
- Age (risk increases with aging)
- Family history and genetic predisposition
- Race and ethnicity (higher prevalence in African Americans)
- Gender (men at higher risk until age 65; women’s risk increases after menopause)
Modifiable Risk Factors
- Dietary Factors: High sodium intake, low potassium intake, excessive alcohol consumption
- Lifestyle Behaviors: Physical inactivity, sedentary lifestyle, smoking
- Weight: Overweight or obesity (BMI ≥25 kg/m²)
- Chronic Stress: Prolonged psychological stress, anxiety
- Comorbid Conditions: Diabetes mellitus, dyslipidemia, chronic kidney disease
- Sleep Disorders: Obstructive sleep apnea, chronic sleep deprivation
- Medication Use: NSAIDs, oral contraceptives, stimulants
As nurses, we focus heavily on modifiable risk factors during patient education and care planning, as these offer the greatest opportunity for patient-driven improvement.
Signs and Symptoms
Subjective Data (Patient-Reported Symptoms)
Most patients with mild to moderate hypertension experience no symptoms at all, which is why routine screening is critical. When symptoms do occur, patients may report:
- Headache, especially occipital (back of head) in the morning
- Dizziness or lightheadedness
- Fatigue or generalized weakness
- Blurred vision or visual disturbances
- Palpitations or sensation of a forceful heartbeat
- Shortness of breath with exertion
- Nosebleeds (epistaxis), though not as common as previously believed
Objective Data (Observable and Measurable Findings)
Nurses assess for the following objective signs during physical examination and monitoring:
- Elevated Blood Pressure Readings: Consistently ≥130/80 mmHg on multiple occasions (BP should be measured in both arms initially; a difference >10 mmHg may indicate vascular disease)
- Cardiovascular Findings:
- Abnormal heart sounds (S4 gallop indicates ventricular stiffness)
- Displaced point of maximal impulse (PMI), suggesting left ventricular hypertrophy
- Irregular heart rhythms (atrial fibrillation is more common with hypertension)
- Retinal Changes: Retinopathy visible on fundoscopic exam (narrowed arterioles, arteriovenous nicking, hemorrhages, or papilledema in severe cases)
- Peripheral Edema: Swelling in the ankles, feet, or sacral area indicating fluid retention
- Weight Gain: Rapid weight gain from fluid retention
- Decreased Urine Output: May indicate kidney dysfunction
Signs of Hypertensive Crisis (Medical Emergency)
Patients experiencing a hypertensive crisis (BP >180/120 mmHg with acute target organ damage) require immediate medical intervention. Red-flag symptoms include:
- Severe, sudden headache
- Severe shortness of breath or respiratory distress
- Chest pain or pressure
- Confusion, altered mental status, or decreased level of consciousness
- Seizures
- Severe anxiety or a sense of impending doom
- Weakness, numbness, or paralysis on one side of the body (stroke symptoms)
- Vision loss or sudden visual changes
- Severe nosebleed that won’t stop
In clinical practice, nurses must recognize these warning signs immediately and activate rapid response protocols.
Nursing Assessment
Comprehensive nursing assessment forms the foundation for accurate nursing diagnosis and effective care planning. Assessment includes subjective and objective data collection, physical examination, laboratory and diagnostic testing, and evaluation for target organ damage.
Health History
Obtain detailed information about:
- Present Symptoms: Duration and severity of any symptoms (headache, dizziness, vision changes)
- Past Medical History: Previous BP readings, duration of hypertension diagnosis, history of cardiovascular disease, stroke, kidney disease, diabetes
- Medication History: Current antihypertensive medications, adherence patterns, side effects; over-the-counter medications and supplements (especially NSAIDs, decongestants)
- Family History: Hypertension, heart disease, stroke, kidney disease, diabetes in first-degree relatives
- Social History:
- Tobacco use (current, former, pack-years)
- Alcohol consumption (quantity, frequency)
- Recreational drug use (cocaine, amphetamines)
- Stress levels and coping mechanisms
- Sleep patterns and quality
- Dietary Assessment: Sodium intake, typical daily meals, processed food consumption, caffeine intake
- Physical Activity: Type, frequency, duration, and intensity of exercise
- Psychosocial Factors: Support systems, financial resources for medications, health literacy, cultural beliefs about health and medication
Physical Examination
Vital Signs:
- Blood Pressure: Measure in both arms using proper technique (patient seated quietly for 5 minutes, arm at heart level, appropriate cuff size). Obtain orthostatic measurements if indicated (especially in older adults or those on multiple antihypertensives).
- Heart Rate and Rhythm: Assess for tachycardia, bradycardia, irregular rhythms
- Respiratory Rate: Assess for tachypnea or dyspnea
- Temperature: Rule out systemic infection or thyroid storm
Anthropometric Measurements:
- Height and weight (calculate BMI)
- Waist circumference (central obesity assessment)
Cardiovascular Examination:
- Palpate peripheral pulses bilaterally (radial, brachial, femoral, dorsalis pedis, posterior tibial)
- Assess capillary refill
- Auscultate heart sounds for murmurs, S3 or S4 gallops, irregular rhythms
- Check for jugular venous distention (JVD)
- Assess for displaced or sustained PMI (indicates left ventricular hypertrophy)
Respiratory Examination:
- Auscultate lung sounds for crackles (pulmonary edema), wheezes
- Assess respiratory effort and use of accessory muscles
Abdominal Examination:
- Auscultate for renal bruits (may indicate renal artery stenosis)
- Palpate for enlarged kidneys or masses
Neurological Examination:
- Assess the level of consciousness, orientation
- Evaluate cranial nerves, motor strength, and sensory function
- Check for focal deficits suggesting previous stroke or transient ischemic attack (TIA)
Integumentary and Extremity Examination:
- Inspect skin color, temperature, and moisture
- Assess for edema (grade pitting edema 1+ through 4+)
- Check for skin breakdown or ulcers (may indicate peripheral vascular disease)
Laboratory and Diagnostic Tests
Routine Laboratory Tests:
- Complete Metabolic Panel (CMP):
- Serum creatinine and blood urea nitrogen (BUN) to assess kidney function
- Estimated glomerular filtration rate (eGFR)
- Electrolytes (sodium, potassium, calcium, chloride, bicarbonate)
- Fasting glucose or hemoglobin A1C (assess for diabetes)
- Lipid Panel: Total cholesterol, LDL, HDL, triglycerides
- Urinalysis: Check for protein (marker of kidney damage), blood, and glucose
- Urine Albumin-to-Creatinine Ratio: Detects early kidney damage
- Thyroid-Stimulating Hormone (TSH): Rule out thyroid disorders
Additional Tests (as indicated):
- Electrocardiogram (ECG/EKG): Assess for left ventricular hypertrophy, arrhythmias, and previous myocardial infarction
- Echocardiogram: Evaluate ventricular size, wall thickness, and ejection fraction
- Chest X-Ray: Assess heart size, pulmonary edema
- 24-Hour Ambulatory Blood Pressure Monitoring: Confirms diagnosis, assesses nocturnal BP patterns
- Renal Ultrasound or CT: Evaluate kidney size, rule out polycystic kidney disease or masses
- Sleep Study: If obstructive sleep apnea is suspected
Assessment for Target Organ Damage
Nurses should systematically assess for evidence of hypertension-related complications affecting major organ systems:
| Organ System | Assessment Parameters | Indicators of Damage |
|---|---|---|
| Cardiovascular | Heart sounds, ECG, echocardiogram, symptoms | Left ventricular hypertrophy, heart failure, coronary artery disease, atrial fibrillation |
| Cerebrovascular | Neurological exam, history of stroke/TIA, cognitive function | Previous stroke, TIA, vascular dementia, cognitive impairment |
| Renal | Creatinine, eGFR, urinalysis, albumin-to-creatinine ratio | Chronic kidney disease (eGFR <60 mL/min/1.73 m²), proteinuria |
| Ocular | Fundoscopic exam, visual acuity, patient-reported vision changes | Hypertensive retinopathy, retinal hemorrhages, papilledema |
| Peripheral Vascular | Peripheral pulses, capillary refill, skin integrity | Peripheral artery disease, claudication, decreased pulses |
Early detection of target organ damage allows for more aggressive treatment and may prevent progression to irreversible complications.
NANDA-I Nursing Diagnoses for Hypertension
Based on comprehensive assessment data, the following nursing diagnoses from the NANDA-I 2024–2026 classification are most commonly applicable to patients with hypertension. These diagnoses guide the development of individualized care plans and prioritize nursing interventions.
1. Decreased Cardiac Output
Related to: Increased afterload (systemic vascular resistance) secondary to chronic hypertension
As evidenced by: Elevated blood pressure, S4 heart sound, fatigue, decreased activity tolerance, dyspnea on exertion
2. Deficient Knowledge
Related to: Lack of exposure to accurate information about hypertension management, unfamiliarity with the disease process
As evidenced by: Verbalization of misconceptions, questions about disease and treatment, non-adherence to medication regimen, inability to explain condition
3. Excess Fluid Volume
Related to: Compromised regulatory mechanisms (sodium retention, kidney dysfunction), excessive sodium intake
As evidenced by: Edema, weight gain, elevated blood pressure, dyspnea, abnormal breath sounds (crackles), jugular venous distention
4. Risk for Unstable Blood Pressure
Risk factors: Inconsistent medication adherence, high-sodium diet, excessive alcohol intake, inadequate knowledge of disease management, non-adherence to treatment plan
5. Sedentary Lifestyle
Related to: Lack of knowledge regarding health benefits of physical activity, insufficient interest in physical activity, lack of motivation
As evidenced by: Physical deconditioning, preference for activities low in physical activity, chooses a daily routine lacking physical exercise
Additional Nursing Diagnoses to Consider:
- Ineffective Health Maintenance: Related to complexity of therapeutic regimen, insufficient knowledge of disease management
- Readiness for Enhanced Self-Health Management: For motivated patients seeking to improve lifestyle and health outcomes
- Activity Intolerance: Related to imbalance between oxygen supply and demand
- Chronic Pain (Headache): Related to increased intracranial pressure secondary to hypertension
- Risk for Decreased Cardiac Tissue Perfusion: Risk factors include hypertension, hyperlipidemia, diabetes
- Anxiety: Related to threat to health status, changes in role functioning
- Ineffective Coping: Related to inadequate resources, high degree of threat from chronic illness
Expected Outcomes and Goals
Nursing goals for patients with hypertension should be measurable, patient-centered, and time-specific, following the NOC (Nursing Outcomes Classification) framework. Goals are categorized into short-term (achievable during hospitalization or within days to weeks) and long-term (achievable over weeks to months).
Short-Term Goals
- Blood pressure reduced to individualized target range (generally <130/80 mmHg) within 24–48 hours of treatment initiation
- Patient verbalizes understanding of hypertension diagnosis and treatment plan before discharge
- Patient demonstrates correct home blood pressure monitoring technique
- Relief or reduction of hypertension-related symptoms (headache, dizziness, dyspnea)
- Patient identifies personal risk factors contributing to hypertension
- Patient states names, purposes, and dosing schedules of prescribed antihypertensive medications
Long-Term Goals
- Maintain blood pressure consistently within target range (<130/80 mmHg for most patients) over 3–6 months
- Achieve and maintain 95% medication adherence as measured by self-report and pharmacy refill records
- Implement and sustain lifestyle modifications for a minimum of 6 months:
- Reduce sodium intake to <2,300 mg daily (or <1,500 mg if recommended)
- Achieve and maintain a healthy body weight (BMI 18.5–24.9 kg/m²)
- Engage in at least 150 minutes of moderate-intensity aerobic exercise weekly
- Limit alcohol to ≤2 drinks/day for men, ≤1 drink/day for women
- Abstain from tobacco use
- No development of new hypertension-related complications (stroke, myocardial infarction, heart failure, chronic kidney disease)
- Demonstrate effective stress management and coping strategies
- Maintain regular follow-up appointments with a healthcare provider every 3–6 months
Nursing Interventions (General)
Before presenting the individualized care plans, the following evidence-based nursing interventions apply broadly to most patients with hypertension:
Blood Pressure Monitoring
- Monitor BP at regular intervals based on clinical status (every 4 hours for acute/unstable patients; daily for stable patients; self-monitoring at home after discharge)
Rationale: Frequent monitoring detects trends, evaluates treatment effectiveness, and identifies hypertensive emergencies early. - Use proper BP measurement technique: Appropriate cuff size, arm at heart level, patient seated quietly for 5 minutes, no talking during measurement, feet flat on the floor
Rationale: Incorrect technique leads to inaccurate readings and inappropriate treatment decisions.
Medication Management
- Administer antihypertensive medications exactly as prescribed (ACE inhibitors, ARBs, beta-blockers, calcium channel blockers, diuretics, alpha-blockers)
Rationale: Each medication class targets different mechanisms of blood pressure regulation; consistent dosing maintains therapeutic levels. - Monitor for medication side effects (orthostatic hypotension, bradycardia, electrolyte imbalances, cough with ACE inhibitors, edema with calcium channel blockers)
Rationale: Early identification of adverse effects allows for timely intervention and medication adjustment. - Assess medication adherence at every encounter; identify barriers (cost, side effects, complexity of regimen, forgetfulness)
Rationale: Non-adherence is a leading cause of uncontrolled hypertension and preventable complications.
Patient Education
- Educate about hypertension pathophysiology in patient-appropriate language
Rationale: Understanding the disease process and its complications increases motivation for self-management. - Teach lifestyle modifications: DASH diet principles, sodium reduction, weight management, physical activity, smoking cessation, stress reduction
Rationale: Lifestyle changes can reduce systolic BP by 10–20 mmHg and may allow reduction in medication doses. - Demonstrate home blood pressure monitoring and ask the patient to perform a return demonstration
Rationale: Home monitoring increases patient engagement, provides additional data for treatment decisions, and identifies white-coat or masked hypertension.
Lifestyle Support
- Encourage regular physical activity: At least 150 minutes weekly of moderate aerobic exercise (brisk walking, swimming, cycling)
Rationale: Regular exercise lowers BP, improves cardiovascular fitness, aids weight loss, and reduces stress. - Promote dietary modifications: Increase fruits, vegetables, whole grains, lean proteins; decrease sodium, saturated fat, processed foods
Rationale: The DASH diet can lower systolic BP by 8–14 mmHg. - Facilitate smoking cessation through counseling, nicotine replacement therapy, and pharmacotherapy referrals
Rationale: Smoking cessation significantly reduces cardiovascular risk; nicotine acutely raises BP and heart rate.
Nursing Care Plans for Hypertension
The following five nursing care plans represent common clinical scenarios encountered in practice. Each care plan includes a specific NANDA-I diagnosis statement with related factors and defining characteristics, measurable expected outcomes, evidence-based interventions with rationales, and evaluation criteria.
Nursing Care Plan 1: Decreased Cardiac Output
Nursing Diagnosis:
Decreased Cardiac Output related to increased afterload secondary to elevated systemic vascular resistance as evidenced by BP 158/96 mmHg, patient reports of fatigue and dyspnea with minimal exertion, S4 heart sound on auscultation, and echocardiogram showing left ventricular hypertrophy.
Expected Outcomes:
- Blood pressure will decrease to the target range (<130/80 mmHg) within 48 hours of initiating or adjusting antihypertensive therapy
- Patient will report a reduction in fatigue and improved activity tolerance within 72 hours
- Heart rate will remain within normal range (60–100 bpm) with regular rhythm
- Patient will deny chest pain, severe dyspnea, or dizziness
- An echocardiogram will show stable or improved left ventricular function within 6 months
Nursing Interventions and Rationales:
- Monitor blood pressure every 4 hours (or more frequently if unstable) using the correct technique in both arms
Rationale: Frequent monitoring identifies BP trends, evaluates medication effectiveness, and detects dangerous elevations early. Bilateral measurement identifies arterial discrepancies suggesting vascular disease. - Assess heart rate, rhythm, and heart sounds every shift; report irregularities or new S3/S4 gallops immediately
Rationale: S4 gallop indicates ventricular stiffness from long-standing hypertension; S3 gallop suggests heart failure. Arrhythmias like atrial fibrillation are common complications of hypertensive heart disease. - Administer prescribed antihypertensive medications on time and monitor response
Rationale: Medications reduce afterload by decreasing vascular resistance (vasodilators, ACE inhibitors, ARBs, calcium channel blockers) and/or reducing fluid volume (diuretics), improving cardiac output and reducing cardiac workload. - Monitor intake and output closely; assess for fluid retention (weight gain, edema, crackles)
Rationale: Fluid overload increases preload and worsens cardiac workload. Daily weights are the most sensitive indicator of fluid balance (1 kg weight change = 1 liter fluid). - Elevate the head of the bed 30–45 degrees if dyspnea or orthopnea are present
Rationale: Semi-Fowler’s position promotes lung expansion, reduces venous return to the heart, decreases pulmonary congestion, and improves oxygenation. - Encourage rest periods between activities; space care activities to prevent fatigue
Rationale: Rest reduces myocardial oxygen demand and cardiac workload, allowing the heart to recover between exertion periods.
Evaluation:
BP decreased to 128/82 mmHg within 36 hours. Patient reports improved energy levels and is able to walk to the bathroom without dyspnea. Heart rate 78 bpm, regular rhythm. S4 gallop is still present, but no new findings. Patient tolerating medication regimen without adverse effects.
Nursing Care Plan 2: Deficient Knowledge (Hypertension Management)
Nursing Diagnosis:
Deficient Knowledge related to unfamiliarity with disease process, treatment regimen, and self-management strategies as evidenced by the patient stating, “I don’t understand why I need medication when I feel perfectly fine,” inability to name current medications or their purposes, and history of missed doses.
Expected Outcomes:
- Patient will explain hypertension and its potential complications in their own words before discharge
- Patient will identify at least four modifiable risk factors for hypertension and personal risk factors by the end of the teaching session
- Patient will correctly name prescribed medications, state their purposes, and identify potential side effects within 24 hours
- Patient will demonstrate proper home blood pressure monitoring technique with 100% accuracy
- Patient will verbalize understanding that hypertension requires treatment even in the absence of symptoms
- The patient will describe warning signs requiring immediate medical attention
Nursing Interventions and Rationales:
- Assess current knowledge level, health literacy, learning readiness, and preferred learning style
Rationale: Baseline assessment establishes an appropriate starting point, prevents repetition of known information, and allows tailoring of teaching methods to individual needs (visual, auditory, kinesthetic). - Provide education on hypertension pathophysiology using simple language and visual aids; explain the “silent killer” concept
Rationale: Understanding that hypertension causes damage even without symptoms increases treatment adherence. Visual aids (diagrams, models) enhance comprehension and retention.
- Review each prescribed medication: name (generic and brand), purpose, dosage, timing, and common side effects; provide written materials
Rationale: Comprehensive medication education improves adherence and helps patients recognize expected versus concerning effects. Written materials reinforce verbal teaching and serve as a reference at home. - Demonstrate home blood pressure monitoring using the patient’s own device; have the patient perform a return demonstration
Rationale: Hands-on practice with immediate feedback ensures competency. Using the patient’s actual equipment identifies device-specific features and troubleshooting needs. - Use teach-back method: “In your own words, tell me why you’re taking this medication.”
Rationale: Teach-back validates comprehension better than asking “Do you understand?” It identifies gaps requiring additional teaching. - Educate on warning signs of hypertensive crisis: severe headache, chest pain, severe dyspnea, vision changes, confusion, weakness
Rationale: Early recognition of emergencies enables timely treatment, potentially preventing stroke, myocardial infarction, or other life-threatening complications.
Evaluation:
Patient demonstrated correct BP monitoring technique and recorded reading in log. Patient stated, “High blood pressure damages my heart and blood vessels even when I don’t feel sick, so I need to take my medicine every day.” Patient correctly named three medications, their purposes, and timing. Verbalized understanding to call 911 for severe headache, chest pain, or trouble breathing.
Nursing Care Plan 3: Excess Fluid Volume
Nursing Diagnosis:
Excess Fluid Volume related to excessive sodium intake (patient reports eating fast food daily) and compromised renal function (creatinine 1.8 mg/dL, eGFR 48 mL/min/1.73 m²) as evidenced by 3 kg weight gain over 5 days, +2 pitting edema bilateral lower extremities, BP 164/100 mmHg, bibasilar crackles, and patient report of dyspnea with exertion.
Expected Outcomes:
- Edema will reduce to trace or absent within 3–5 days of treatment
- Weight will decrease by 2–3 kg within 72 hours (return to baseline dry weight)
- Blood pressure will decrease to <140/90 mmHg within 48 hours
- Lung sounds will be clear to auscultation bilaterally
- Intake and output will be balanced (output may exceed intake initially with diuresis)
- Patient will verbalize understanding of sodium restriction and demonstrate ability to read food labels
Nursing Interventions and Rationales:
- Monitor daily weights at the same time each morning (after voiding, before breakfast, same scale, same clothing)
Rationale: Daily weights are the most accurate indicator of fluid status. Consistency in timing and conditions ensures reliable comparison. Weight gain of 1 kg = 1 liter of retained fluid. - Assess edema location and severity using the pitting scale; measure leg circumference if significant edema is present
Rationale: Systematic edema assessment tracks treatment response. Dependent edema (ankles, sacrum) indicates fluid volume excess. Circumference measurements provide objective data. - Auscultate lung sounds every shift; report crackles, wheezes, or diminished sounds
Rationale: Crackles (rales) indicate pulmonary edema from fluid overload—a sign of worsening heart failure or severe fluid retention requiring immediate intervention. - Administer prescribed diuretics (furosemide, hydrochlorothiazide, spironolactone) as ordered; monitor for therapeutic effect and side effects
Rationale: Diuretics promote sodium and water excretion, reducing blood volume, decreasing preload and afterload, and lowering blood pressure. Different classes have different mechanisms and side effect profiles. - Monitor electrolytes (especially potassium, sodium) and renal function (creatinine, BUN) daily or as ordered
Rationale: Diuretics can cause hypokalemia (loop and thiazide diuretics) or hyperkalemia (potassium-sparing diuretics), both dangerous. Aggressive diuresis may worsen renal function. - Restrict sodium intake to <2,000 mg daily; collaborate with a dietitian for meal planning
Rationale: Dietary sodium restriction prevents further fluid retention and enhances diuretic effectiveness. A dietitian’s expertise helps create realistic, culturally appropriate meal plans. - Educate the patient on reading nutrition labels to identify sodium content; provide list of high-sodium foods to avoid
Rationale: Empowering patients to make informed food choices promotes long-term adherence. Processed foods, canned soups, deli meats, and restaurant meals are often extremely high in sodium.
Evaluation:
Weight decreased by 2.5 kg over 3 days. Edema reduced to trace in bilateral ankles. BP improved to 136/86 mmHg. Lung sounds clear bilaterally. Patient demonstrated ability to read food labels and identify high-sodium items. Patient states, “I’m going to cook more at home instead of eating out.”
Nursing Care Plan 4: Risk for Unstable Blood Pressure
Nursing Diagnosis:
Risk for Unstable Blood Pressure
Risk Factors: Inconsistent medication adherence (patient admits forgetting evening dose 3–4 times weekly), excessive dietary sodium intake (fast food consumption, processed snacks), stressful work environment with inadequate coping strategies, and limited understanding of the relationship between lifestyle factors and blood pressure control.
Expected Outcomes:
- Blood pressure will remain stable within the target range (<130/80 mmHg) with variability <10 mmHg between readings
- Patient will achieve 95% medication adherence over 2 weeks as documented in the medication log
- Patient will implement at least two stress-reduction techniques daily
- Patient will limit sodium intake to <2,300 mg daily
- Patient will identify personal triggers for blood pressure fluctuation
- Patient will not develop hypertensive urgency or emergency during the care period
Nursing Interventions and Rationales:
- Monitor blood pressure at consistent times throughout the day (morning, midday, evening) to establish patterns
Rationale: BP naturally varies throughout the day (circadian rhythm). Pattern identification helps determine optimal medication timing and identifies triggers for spikes or drops. - Collaborate with the patient to develop a medication reminder system (phone alarms, pill organizer, linking to daily routine)
Rationale: Consistent medication timing maintains stable therapeutic drug levels, preventing peaks and troughs in BP control. Personalized reminders increase adherence. - Review current medication regimen with pharmacist; consider once-daily formulations if adherence is an issue
Rationale: Simplifying regimens improves adherence. Combination medications reduce pill burden. Pharmacist expertise ensures optimal medication selection and timing. - Teach the relationship between lifestyle factors and BP: sodium increases fluid retention; stress activates the sympathetic nervous system; caffeine causes vasoconstriction
Rationale: Understanding cause-and-effect relationships empowers patients to make informed choices. Awareness of personal triggers enables proactive management. - Instruct on stress-reduction techniques: deep breathing exercises, progressive muscle relaxation, mindfulness meditation, guided imagery
Rationale: Chronic stress elevates cortisol and activates the sympathetic nervous system, increasing heart rate and vascular resistance. Relaxation techniques lower BP by 5–10 mmHg. - Limit caffeine intake to <200 mg daily (approximately 2 cups of coffee); avoid energy drinks
Rationale: Caffeine acutely raises BP through sympathetic stimulation and vasoconstriction. Large doses or sudden increases can trigger dangerous spikes. - Coordinate multidisciplinary care: dietitian for meal planning, social worker for stress/financial resources, pharmacist for medication optimization
Rationale: A comprehensive team approach addresses multiple contributing factors simultaneously. Social support and resources improve adherence and outcomes.
Evaluation:
Blood pressure readings remained between 124/76 mmHg and 132/84 mmHg over a 10-day period. Patient demonstrated use of phone alarm for medication reminders and reports only one missed dose in the past week. Patient practiced deep breathing exercises twice daily and reports feeling “less overwhelmed.” Sodium intake decreased to an estimated 2,400 mg daily (still working toward goal but improved from baseline >4,000 mg).
Nursing Care Plan 5: Sedentary Lifestyle
Nursing Diagnosis:
Sedentary Lifestyle related to insufficient knowledge regarding health benefits of physical activity and lack of motivation as evidenced by patient report of no regular exercise (“I sit at a desk all day and just watch TV at night”), BMI of 32 kg/m², and physical deconditioning noted during assessment (dyspnea after walking 50 feet).
Expected Outcomes:
- Patient will verbalize understanding of the relationship between physical activity and blood pressure control within 24 hours
- Patient will identify three personal barriers to exercise and develop strategies to overcome each barrier
- Patient will initiate low-impact physical activity (walking) for 10–15 minutes daily within 1 week
- Patient will gradually increase activity duration to 30 minutes most days of the week over 3 months
- Patient will demonstrate improved exercise tolerance (able to walk 10 minutes without dyspnea) within 4 weeks
- Patient will lose 0.5–1 kg per week through combined dietary changes and increased activity
Nursing Interventions and Rationales:
- Assess current activity level, exercise preferences, past exercise history, and physical limitations
Rationale: Baseline assessment identifies the starting point and helps select activities the patient is likely to enjoy and sustain. Identifying preferences increases adherence; addressing limitations prevents injury. - Educate on cardiovascular benefits of regular physical activity: lowers BP by 5–8 mmHg, improves insulin sensitivity, aids weight loss, reduces stress, and strengthens the heart
Rationale: Understanding concrete health benefits increases intrinsic motivation. Regular aerobic exercise provides BP reduction comparable to adding a medication. - Collaborate with the patient to set realistic, incremental activity goals using the SMART framework (Specific, Measurable, Achievable, Relevant, Time-bound)
Rationale: Small, achievable goals build confidence and prevent discouragement. The SMART framework ensures goals are clear and measurable, facilitating evaluation. - Start with low-impact activities the patient enjoys: walking, swimming, cycling, water aerobics, gardening
Rationale: Enjoyment is the strongest predictor of long-term adherence. Low-impact activities reduce injury risk, especially in deconditioned or overweight individuals. - Encourage incorporating activity into daily routine: parking farther away, taking stairs, walking during lunch break, and evening family walks
Rationale: Integration into daily life is more sustainable than adding separate “exercise time.” Environmental modifications make activity the easy choice. - Provide community resources for safe, accessible exercise: local walking groups, senior centers, YMCA programs, cardiac rehabilitation if indicated
Rationale: Social support enhances motivation and accountability. Structured programs provide guidance, safety, and community connection. Removing barriers (cost, location, knowledge) increases participation. - Monitor heart rate and blood pressure response to activity; teach patient to assess exertion using Rate of Perceived Exertion (RPE) or talk test
Rationale: Monitoring physiologic response ensures exercise intensity is safe and effective (target: moderate intensity, able to talk but not sing). Excessive exertion can dangerously elevate BP in poorly controlled hypertension.
Evaluation:
Patient stated, “I didn’t realize that walking 30 minutes a day could lower my blood pressure as much as medication.” Identified barriers: lack of time, fatigue after work, and safety concerns in the neighborhood. Solutions developed: walk during lunch break at work, join a coworker walking group, walk in the local mall in the evenings. Began walking 15 minutes daily for past 5 days. Reports feeling “more energetic” and “sleeping better.” BP improved from 158/94 mmHg to 146/88 mmHg after 2 weeks of combined medication and activity changes.
Patient and Family Education
Effective patient education is fundamental to successful hypertension management. As nurses, we translate complex medical information into understandable, actionable guidance. Education should be ongoing, reinforced at every encounter, and tailored to individual learning needs.
Understanding Hypertension
Key Teaching Points:
- “Your blood pressure is the force of blood pushing against your artery walls. When this force stays too high for too long, it damages your blood vessels, heart, kidneys, and brain.”
- “Hypertension is called the ‘silent killer’ because you usually can’t feel it, but it’s causing harm inside your body every day.”
- “Even though you might feel fine, uncontrolled high blood pressure significantly increases your risk of heart attack, stroke, heart failure, kidney failure, and vision loss.”
- “The good news is that hypertension can be controlled through medication and lifestyle changes, greatly reducing your risk of complications.”
Medication Adherence
Essential Education:
- Take medications exactly as prescribed, even when feeling well. Never stop suddenly without consulting your healthcare provider.
- Common medication classes and what to expect:
- Diuretics (“water pills”): Increase urination; take in the morning to avoid nighttime bathroom trips
- ACE inhibitors/ARBs: May cause dry cough (ACE inhibitors); report if persistent
- Beta-blockers: May cause fatigue initially; don’t stop suddenly (can cause rebound hypertension)
- Calcium channel blockers: May cause ankle swelling; report if severe
- Report side effects to your provider rather than stopping medication on your own
- Use reminder systems: Pill organizers, phone alarms, linking to daily routines (breakfast, bedtime)
- Refill prescriptions on time; don’t run out of medication
- Discuss cost concerns with your provider; generic alternatives and assistance programs are often available
Dietary Modifications (DASH Diet)
DASH (Dietary Approaches to Stop Hypertension) Diet Principles:
Foods to Increase:
- Fruits and vegetables: 8–10 servings daily
- Whole grains: Brown rice, whole wheat bread, oatmeal, quinoa
- Lean proteins: Skinless poultry, fish, beans, lentils, tofu
- Low-fat dairy: Skim milk, low-fat yogurt, reduced-fat cheese
- Nuts, seeds, and healthy fats: Almonds, walnuts, olive oil, avocado
- Potassium-rich foods: Bananas, oranges, potatoes, spinach, tomatoes
Foods to Limit or Avoid:
- Sodium: Limit to <2,300 mg daily (or <1,500 mg if recommended). Avoid adding salt at the table, reduce salt in cooking, avoid processed foods, canned soups, deli meats, frozen dinners, salty snacks, and restaurant meals.
- Saturated and trans fats: Red meat, full-fat dairy, fried foods, baked goods
- Added sugars: Sugary drinks, desserts, candy
- Alcohol: Limit to ≤2 drinks/day for men, ≤1 drink/day for women
Practical Tips:
- Read nutrition labels: Choose products with <140 mg sodium per serving
- Cook at home more often; restaurant meals are typically very high in sodium
- Use herbs, spices, lemon, and garlic instead of salt for flavoring
- Rinse canned vegetables to remove excess sodium
- Choose fresh or frozen vegetables over canned ones
Physical Activity
Recommendations:
- Goal: At least 150 minutes of moderate-intensity aerobic exercise weekly (e.g., 30 minutes most days)
- Good choices: Brisk walking, swimming, cycling, dancing, water aerobics, yard work
- Start slowly if currently inactive; even 10-minute sessions provide benefit
- Warm up and cool down to prevent injury
- Stop and seek help if you experience chest pain, severe shortness of breath, dizziness, or palpitations during exercise
Home Blood Pressure Monitoring
Technique:
- Use a validated, upper-arm cuff device (avoid wrist or finger monitors)
- Measure at the same times each day (morning before medications, evening before dinner)
- Sit quietly for 5 minutes before measuring
- Sit with back supported, feet flat on the floor, arm at heart level
- Don’t talk during measurement
- Take 2–3 readings 1 minute apart; record all results
- Bring your log to all appointments
When to Call Your Provider:
- Readings consistently above your target range
- Readings >180/120 mmHg (hypertensive urgency)
- New or worsening symptoms
Lifestyle Modifications
Smoking Cessation:
- Nicotine raises blood pressure and heart rate
- Smoking damages blood vessels and increases heart attack/stroke risk
- Resources: Quitline (1-800-QUIT-NOW), nicotine replacement therapy, medications (varenicline, bupropion), counseling
Alcohol Moderation:
- Excessive alcohol raises blood pressure
- Limit to ≤2 drinks/day for men, ≤1 drink/day for women
- One drink = 12 oz beer, 5 oz wine, or 1.5 oz spirits
Stress Management:
- Chronic stress contributes to high blood pressure
- Effective techniques: Deep breathing, meditation, yoga, regular exercise, adequate sleep, hobbies, social connection
- Consider counseling if stress or anxiety is overwhelming
Weight Management:
- Every 10 pounds of weight loss can reduce systolic BP by 5–20 mmHg
- Aim for gradual weight loss (0.5–1 kg per week) through diet and activity changes
- Focus on sustainable lifestyle changes, not extreme diets
Warning Signs Requiring Immediate Medical Attention
Call 911 or go to the emergency room immediately for:
- Severe headache (worst headache of your life)
- Chest pain or pressure
- Severe shortness of breath
- Sudden weakness, numbness, or difficulty speaking (stroke symptoms)
- Severe anxiety or sense of doom
- Vision loss or sudden vision changes
- Blood pressure >180/120 mmHg with symptoms
- Seizures
Follow-Up Care
- Keep all scheduled appointments with your healthcare provider
- Typical follow-up schedule: Every 3–6 months once BP is controlled; more frequently if uncontrolled or medications are being adjusted
- Annual monitoring: Kidney function tests, cholesterol panel, urine protein, eye exam
- Report new symptoms promptly rather than waiting for a scheduled appointment
Frequently Asked Questions
Is hypertension a NANDA nursing diagnosis?
No, hypertension itself is not a NANDA nursing diagnosis—it is a medical diagnosis made by a physician or other licensed healthcare provider based on objective blood pressure measurements and diagnostic criteria. However, nurses use NANDA-I nursing diagnoses to describe the human responses to hypertension and guide nursing care planning.
Common NANDA-I nursing diagnoses for patients with hypertension include:
- Decreased Cardiac Output (related to increased afterload)
- Deficient Knowledge (related to disease management)
- Excess Fluid Volume (related to sodium retention)
- Risk for Unstable Blood Pressure (risk diagnosis)
- Sedentary Lifestyle (related to physical inactivity)
Nursing diagnoses focus on problems that nurses can independently treat through nursing interventions, whereas medical diagnoses require physician orders for treatment (medications, procedures).
What is an example of a nursing diagnosis for hypertension?
A complete nursing diagnosis statement includes three components: the diagnosis label (from NANDA-I), related factors (the cause or contributing factors), and defining characteristics (the evidence or “as evidenced by” signs and symptoms).
Example:
Deficient Knowledge related to unfamiliarity with disease process and treatment regimen as evidenced by the patient stating “I don’t know why I need to take medication when I feel fine,” inability to name current medications, and history of missed medication doses.
This diagnosis guides nursing interventions focused on patient education, teach-back methods, medication counseling, and providing resources for self-management.
Which nursing diagnosis is the priority for a patient with a hypertensive crisis?
For a patient experiencing hypertensive crisis (BP >180/120 mmHg with acute target organ damage), the priority nursing diagnosis is:
Risk for Decreased Cardiac Tissue Perfusion or Risk for Ineffective Cerebral Tissue Perfusion
Rationale: Hypertensive crisis is a medical emergency requiring immediate intervention to lower blood pressure in a controlled manner and prevent life-threatening complications such as stroke, myocardial infarction, heart failure, or kidney injury. The priority is preserving tissue perfusion to vital organs.
Priority nursing actions include:
- Activate rapid response or call the provider immediately
- Continuously monitor blood pressure and cardiac rhythm
- Administer IV antihypertensive medications as ordered (nitroprusside, nicardipine, labetalol)
- Maintain patent IV access
- Perform frequent neurological assessments
- Monitor for signs of stroke, myocardial infarction, or pulmonary edema
- Reduce environmental stimuli and promote a calm environment
- Prepare for possible ICU admission
Remember: In hypertensive urgency (BP >180/120 without symptoms or organ damage), the priority is different—gradual BP reduction over 24–48 hours with oral medications rather than aggressive IV treatment.
What are the most common antihypertensive medications nursing students should know for the NCLEX?
Nursing students should be familiar with the major classes of antihypertensive medications, their mechanisms, common side effects, and nursing considerations:
- Diuretics (Thiazides: hydrochlorothiazide; Loop: furosemide; Potassium-sparing: spironolactone)
- Action: Decrease blood volume by promoting sodium and water excretion
- Side effects: Hypokalemia (thiazides and loop), hyperkalemia (potassium-sparing), orthostatic hypotension, dehydration
- Nursing: Monitor electrolytes, daily weights, I&O; teach to take in the morning
- ACE Inhibitors (lisinopril, enalapril, ramipril—end in “-pril”)
- Action: Block conversion of angiotensin I to angiotensin II, reducing vasoconstriction
- Side effects: Dry cough, hyperkalemia, angioedema (rare but serious)
- Nursing: Monitor potassium, teach about cough, assess for angioedema
- Angiotensin II Receptor Blockers (ARBs) (losartan, valsartan—end in “-sartan”)
- Action: Block angiotensin II receptors, preventing vasoconstriction
- Side effects: Hyperkalemia, dizziness; less likely to cause cough than ACE inhibitors
- Nursing: Similar to ACE inhibitors; often used if the patient can’t tolerate ACE inhibitors
- Calcium Channel Blockers (amlodipine, diltiazem, verapamil)
- Action: Prevent calcium entry into vascular smooth muscle, causing vasodilation
- Side effects: Peripheral edema (especially amlodipine), constipation (verapamil), bradycardia
- Nursing: Monitor heart rate, assess for edema, teach about constipation
- Beta-Blockers (metoprolol, atenolol, carvedilol—end in “-olol”)
- Action: Block beta-adrenergic receptors, decreasing heart rate and contractility
- Side effects: Bradycardia, fatigue, bronchospasm (avoid in asthma)
- Nursing: Monitor heart rate (hold if <60 bpm per protocol), teach not to stop suddenly
How do you explain hypertension to a patient or family member?
In simple, patient-friendly language:
“Think of your blood vessels like garden hoses carrying blood throughout your body. Your blood pressure is the force of blood pushing against the walls of those hoses. When this force stays too high for too long, it damages the hoses, making them stiff and weak.
High blood pressure is dangerous because you usually can’t feel it happening—that’s why we call it the ‘silent killer.’ But inside your body, it’s putting extra strain on your heart (making it work harder), damaging your blood vessels, and increasing your risk of heart attacks, strokes, and kidney problems.
The good news is that we can control high blood pressure with medication and healthy lifestyle changes, such as eating less salt, exercising regularly, maintaining a healthy weight, and managing stress. Taking your medication every day—even when you feel fine—is extremely important because it helps protect your heart, brain, and kidneys from damage.
We’ll work together as a team to get your blood pressure to a healthy level and keep it there. I’m here to answer your questions and help you every step of the way.”
References
- Ackley, B. J., Ladwig, G. B., Makic, M. B., Martinez-Kratz, M. R., & Zanotti, M. (2023). Nursing diagnoses handbook: An evidence-based guide to planning care. St. Louis, MO: Elsevier.
- Egan BM, Zhao Y, Axon RN. US trends in prevalence, awareness, treatment, and control of hypertension, 1988-2008. JAMA. 2010 May 26;303(20):2043-50. doi: 10.1001/jama.2010.650. PMID: 20501926.
- Harding, M. M., Kwong, J., & Hagler, D. (2022). Lewis’s Medical-Surgical Nursing: Assessment and Management of Clinical Problems, Single Volume. Elsevier.
- Herdman, T. H., Kamitsuru, S., & Lopes, C. (2024). NANDA International Nursing Diagnoses – Definitions and Classification, 2024-2026.
- Ignatavicius, D. D., Rebar, C., & Heimgartner, N. M. (2023). Medical-Surgical Nursing: Concepts for Clinical Judgment and Collaborative Care. Elsevier.
- Oparil S. Women and hypertension: what did we learn from the Women’s Health Initiative? Cardiol Rev. 2006 Nov-Dec;14(6):267-75. doi: 10.1097/01.crd.0000240530.94242.0c. PMID: 17053372.
- Muntner P, Hardy ST, Fine LJ, Jaeger BC, Wozniak G, Levitan EB, Colantonio LD. Trends in Blood Pressure Control Among US Adults With Hypertension, 1999-2000 to 2017-2018. JAMA. 2020 Sep 22;324(12):1190-1200. doi: 10.1001/jama.2020.14545. PMID: 32902588; PMCID: PMC7489367.
- Silvestri, L. A. (2023). Saunders comprehensive review for the NCLEX-RN examination. St. Louis, MO: Elsevier.